Sleep Hygiene
Good sleep is essential for brain recovery after concussion. The following practical sleep hygiene tips are intended to support rest and reduce symptoms. If symptoms persist or worsen, contact your clinician.
Before bed
Keep a regular sleep schedule: go to bed and wake up at the same times each day, including weekends. Consistency helps reset the brain’s internal clock.
Wind down early: allow 30–60 minutes of calm, low-stimulation activities before bed (reading a book with soft lighting, gentle stretching, breathing exercises). Avoid mentally demanding tasks.
Limit screen exposure: stop using phones, tablets, computers and TV at least 60–90 minutes before sleep. Screens emit blue light that disrupts melatonin and can worsen symptoms. If unavoidable, use blue-light filters and reduce brightness.
Manage light and sound: dim lights in the hour before bed and make your bedroom quiet and dark at bedtime. Use blackout curtains, eye masks or earplugs if needed.
Avoid stimulants and alcohol: do not use caffeine, nicotine or energy drinks in the afternoon and evening. Avoid alcohol close to bedtime — it fragments sleep architecture and can impede recovery.
Mind food and fluids: have your last large meal at least 2–3 hours before bed. Reduce fluids in the evening to minimise night-time toilet trips.
Bedroom environment
Keep the bedroom for sleep only: do work, study, or symptom-provoking tasks elsewhere so the brain associates the bedroom with rest.
Comfortable temperature: maintain a cool, comfortable room
Return to sport
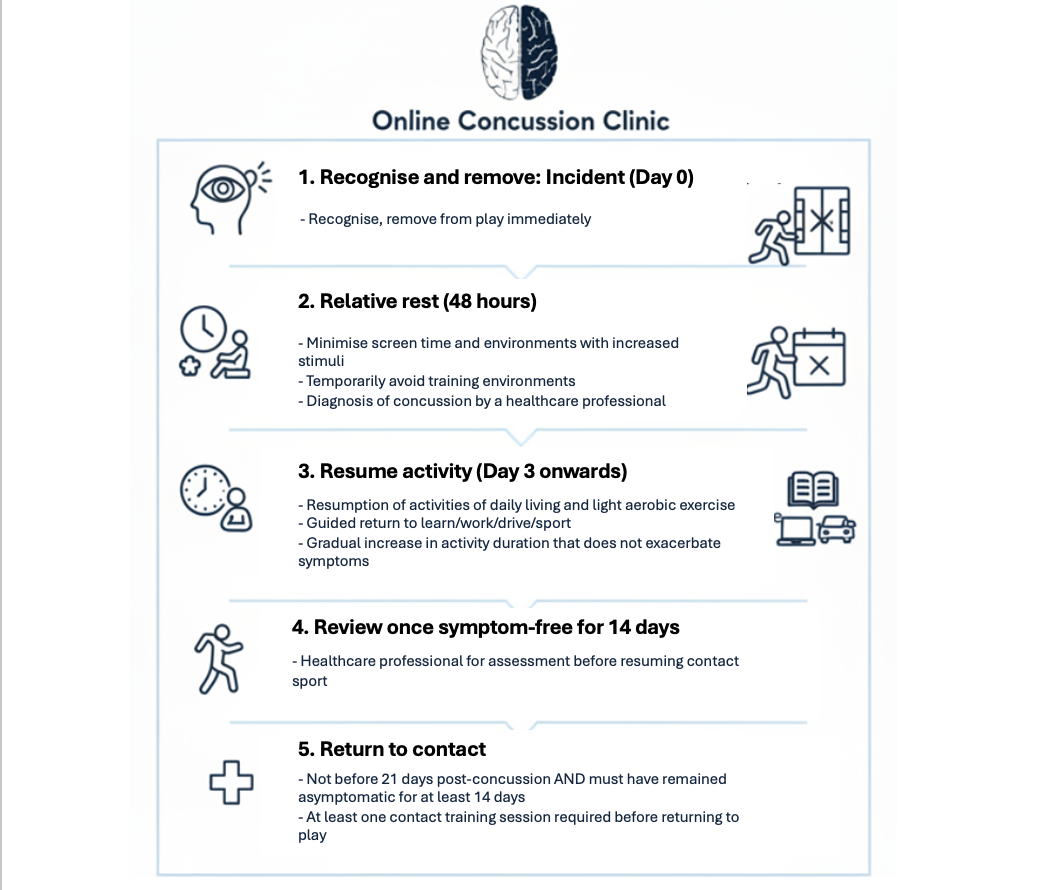
Returning to contact sport after a concussion should follow a structured, individualised graded return-to-play protocol under the guidance of a clinician experienced in concussion management; athletes must complete a progressive exertion program without significant symptom exacerbation, and demonstrate normal balance, cognition and sport-specific skills before contact is reintroduced.
Clearance should be based on objective assessment where possible (neurocognitive testing if indicated, vestibular/oculomotor exam, and balance testing) alongside clinical judgement, with extra caution for adolescents and those with previous concussions who have longer recovery trajectories.
Protection strategies, communication with coaches and schools, and a plan for immediate removal from play if symptoms recur are essential; when in doubt, delay return—premature return to contact increases the risk of prolonged recovery and repeat injury.